WHAT TO EXPECT AT HYSTEROSALPINGOGRAPHY (HSG) PROCEDURE
If you know what to expect at hysterosalpingography(HSG) procedure, it will be better tolerated. Hysterosalpingography is a radiological investigation that is done using water soluble iodinated contrast or, iodinated oil to evaluate the cervix, womb and fallopian tubes.

INDICATIONS FOR HYSTEROSALPINGOGRAPHY
Hysterosalpingography might be requested by the gynaecologist in the following situation;
- Women who are unable to conceive.
- Women of reproductive age with abnormal menstrual bleeding like loss of menses when the woman is not pregnancy.
- Women with mid-trimester pregnancy loss suspected to be due to the inability of the cervix to hold pregnancy till maturity.
- Women with recurrent pregnancy loss from suspected abnormality of the womb.
CONTRA-INDICATIONS TO HYSTEROSALPINGOGRAPHY
HSG is not done in the following situation;
- Confirmed pregnancy
- During menses
- Recent uterine or tubal surgery
- Infection; HSG in the presence of active vaginal or cervical infection can result in transferring the offending pathogen into the upper genital tract and the pelvis.
WHEN SHOULD HYSTEROSALPINGOGRAPHY PROCEDURE BE DONE
The procedure is done after menses within the 6th to 12th day from the first day of the menstrual flow. This period of the menstrual cycle is chosen for the procedure to avoid disrupting an ongoing pregnancy. Also, it gives better visualization of the cavity of the womb as the endometrium, the inner most layer of the womb, is thinnest at this time. Women who have lost their menses and are being evaluated for infertility, might be made to menstruate. The procedure can then be done at the stated time above. It can also be done for women who have lost their menses but have a negative result for pregnancy.
HYSTEROSALPINGOGRAPHY(HSG) PROCEDURE
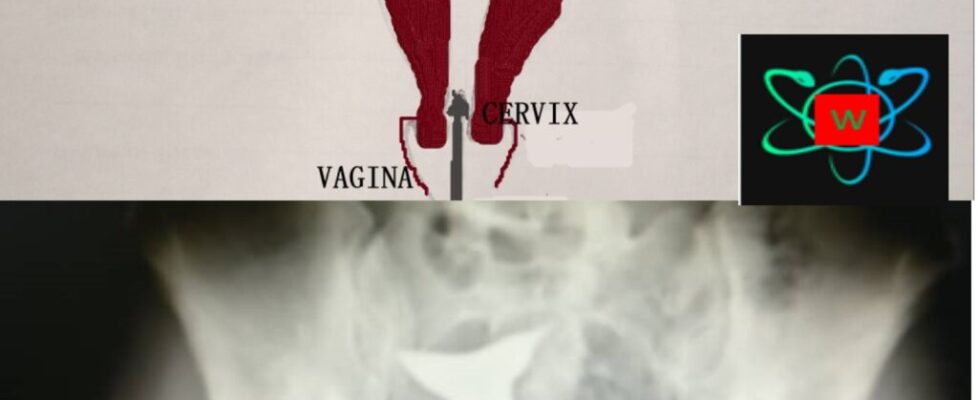
Most women describe the hysterosalpingography(HSG) procedure to be extremely painful and dreadful. Why is that so? maybe they were not given pain medication. Thus, pain medication is required before the procedure. This can be given about 30 to 60minutes before the procedure. After changing into a procedure robe, an x-ray film called the scout film is taken while the woman is lying on the back (supine position). The patient is repositioned with the hip and knee bent and thighs apart. The vulva and vagina is cleaned with antiseptic solution. A plastic or metal instrument, speculum, will be inserted into the vagina. The speculum is open to expose the cervix. The cervix is also cleaned with antiseptic solution. Another instrument, catheter or cannula of appropriate size, will be inserted into the cervix. It is through this that the contrast will be injected slowly through the cervix, womb, fallopian tubes and into the pelvis. Then more x-ray films will be taken. Sometimes a repeat film can be taken if the first taken for a particular position is not good enough for interpretation.
INTERPRETATION OF HYSTEROSALPINGOGRAPHY FILM
The scout film is taken to serve as a reference film. The contrast is meant to outline the upper reproductive tract. If the contrast outlines the fallopian tubes and spills into the pelvis, the tubes are patent. When the contrast does not outline the fallopian tube; it is either tubal spasm or blockade. When the end of the contrast tapers into the tube but does not spill, it is tubal spasm. However, when the end of the contrast is rounded, it is tubal occlusion. The presence of fibroid or polyps in the womb will appear as a filling defect. The internal diameter of the cervix can also be measured. It will be dilated when the cervix is incompetent.
COMPLICATIONS OF HYSTEROSALPINGOGRAPHY
- Bleeding; this occur due to injury to the cervix by the instruments used
- Allergic reaction to contrast; might manifest as chills and rigor, wheals, confusion or even loss of consciousness. Do not worry as this is not very common. Even if it occurs, there are emergency medication in the procedure room to arrest the situation.
- Pain; this can occur during the procedure when the instruments are introduced into the genital tract or when the contrast is injected. After the procedure, pain can occur from uterine spasm. This is usually short live and can be taken care of by the use of pain medication. However, when this pain persists with associated fever and foul-smelly vaginal discharge then, you need to see the gynaecologist at the emergency room.
- Pelvic infection; this can result in pelvic inflammatory disease as the offending pathogen is introduce to the upper reproductive tract from the lower reproductive tract.
- Vasovagal reaction; manifest as fainting attack following manipulation of the cervix, insertion of the cannula or catheter.